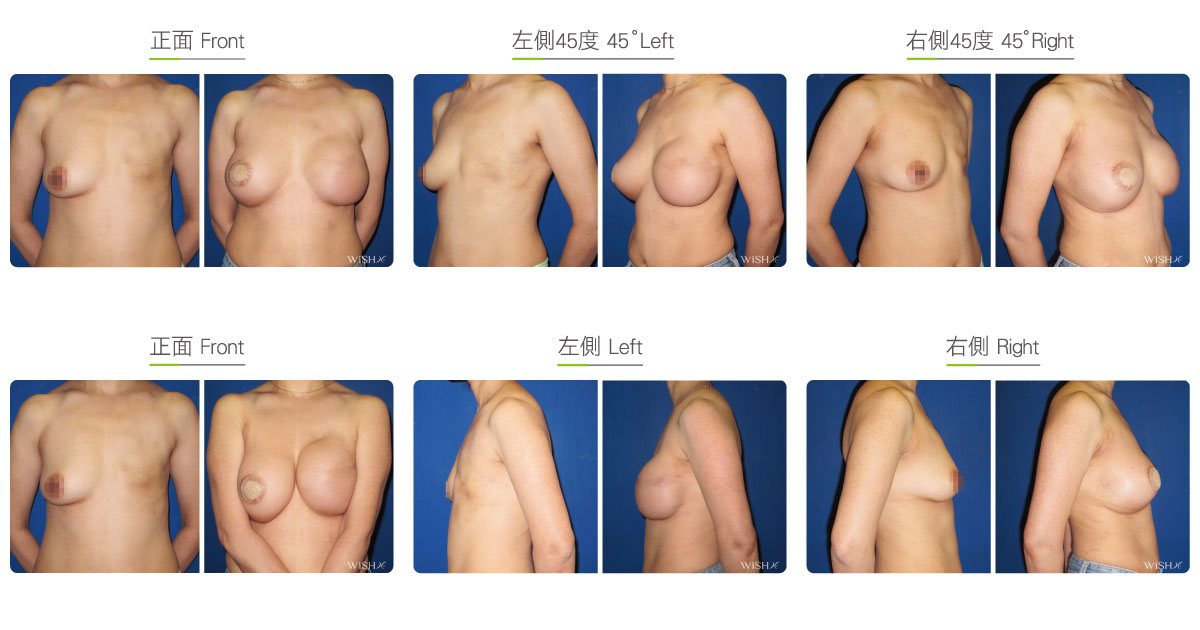
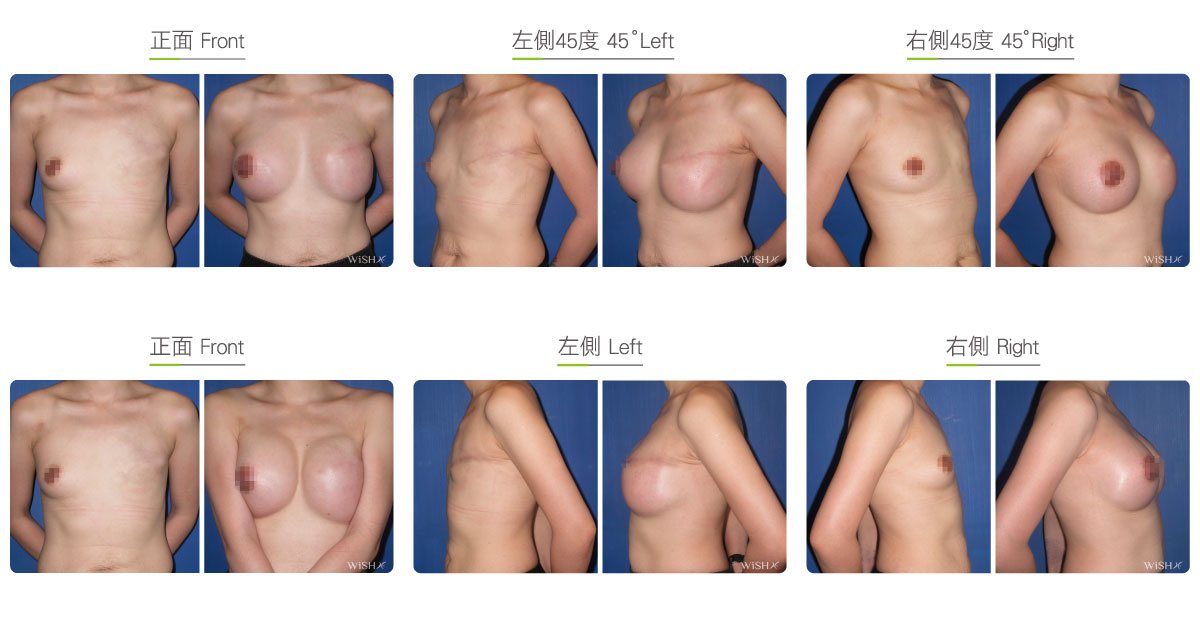
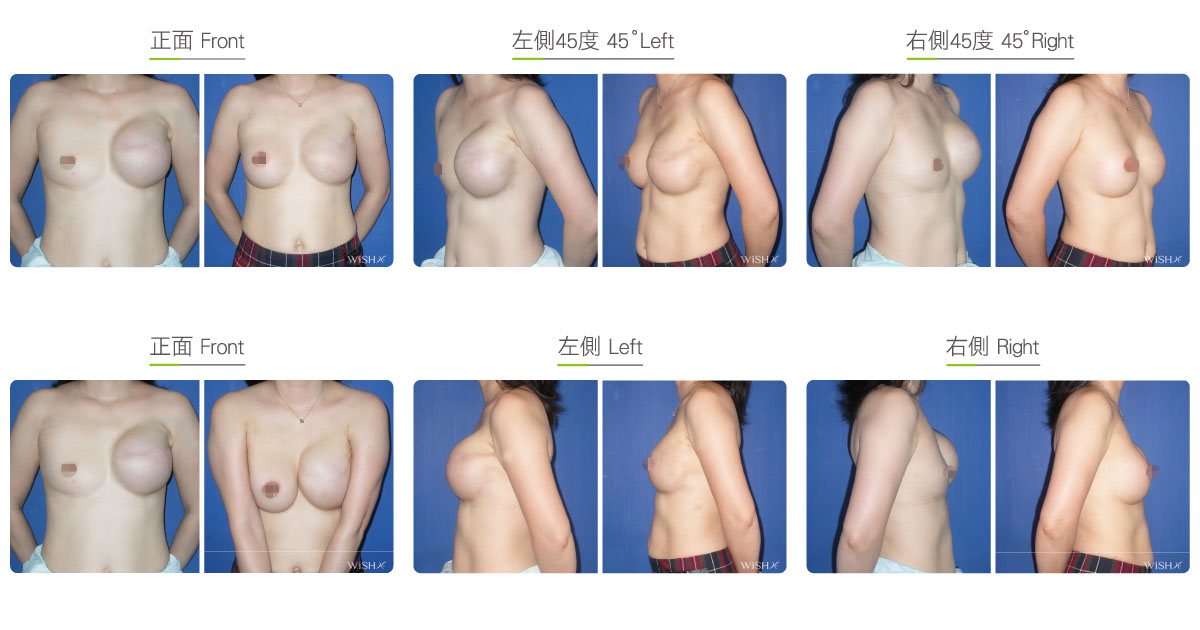
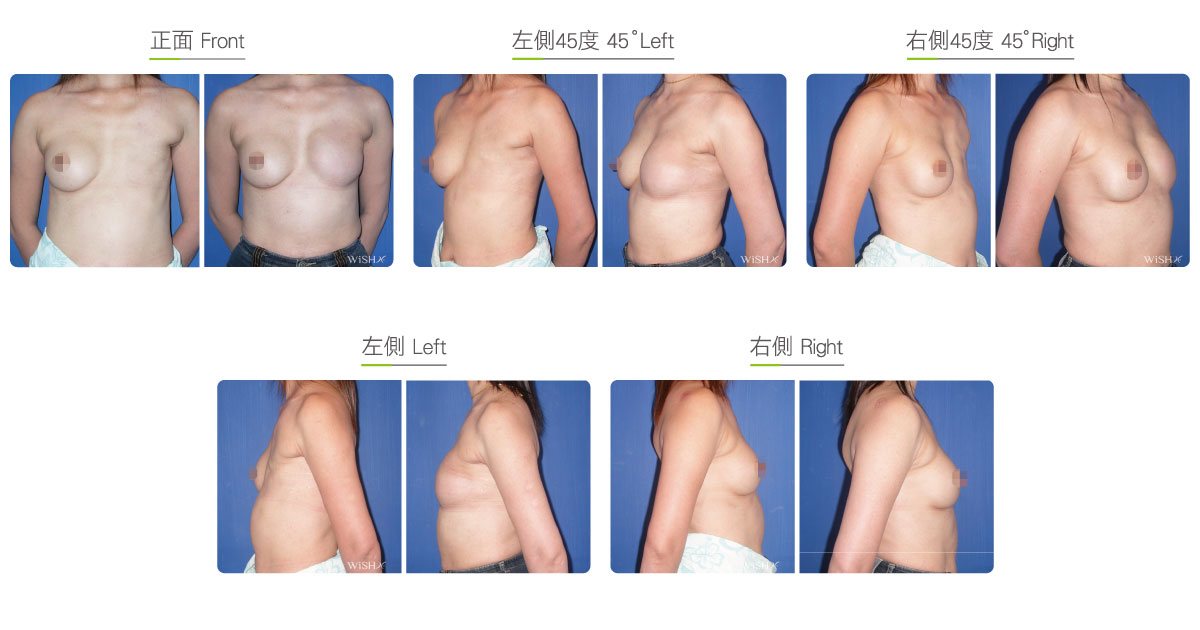
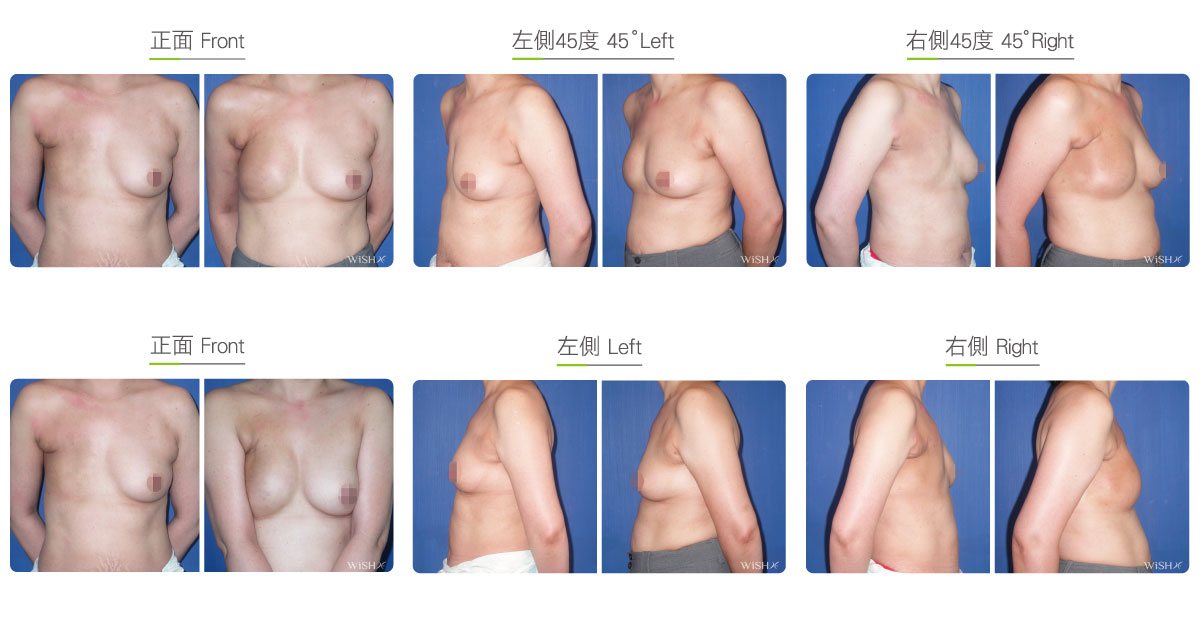
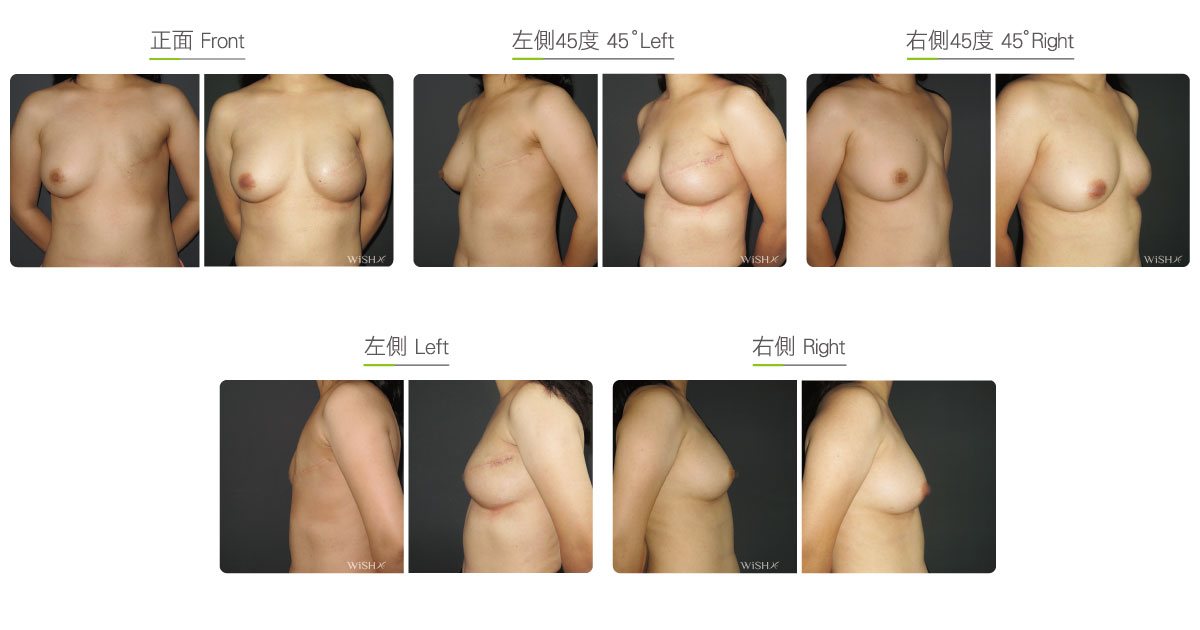
Two-stage Reconstruction
One-stage reconstruction with implants is not recommended for those who underwent subtotal mastectomy, total mastectomy, radiation therapy, or chemotherapy because the skin of the affected breast is thinner, tighter, or even fibrotic. It is more likely to lead to complications such as capsular contracture, implant deformity, poor wound healing, wound infection, or even implant extrusion. To ensure the safety and effectiveness of breast reconstruction, these patients should consider the two-stage procedure:
- Stage 1 Tissue expansion with a saline inflated expander
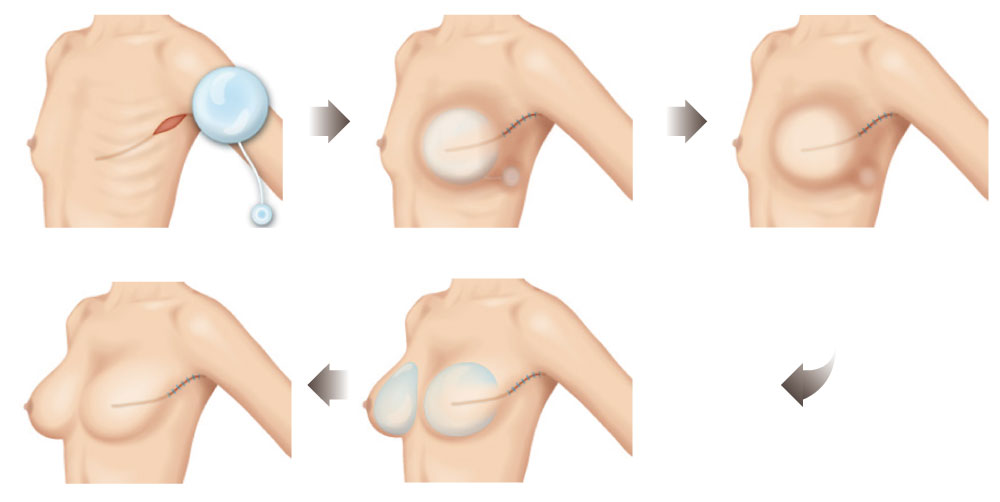
The affected breast would have a temporary tissue expander for 3 months. Dr. Chuang makes a 3–4-cm incision along an original scar, dissects through the subcutaneous space with an endoscope and ESUs, and places a saline tissue expander to maintain the pocket. An internal port connected with the expander is planted in the skin to inject saline solution periodically. By inflation of tissue expander, the skin tension and elasticity can be gradually increased to create a larger pocket for a breast implant. Dr. Chuang has adopted a new incision and surgery of rapid expansion and can fill 50%–70% of the volume during tissue expander placement. This method allows the rapid expansion of the subcutaneous space and a shortened period of waiting during reconstruction. Patients would only need to revisit once a month for a saline injection, unlike traditional surgeries that require frequent hospital visits for more times of injection, which increase patient discomfort and infection risk. With Dr. Chuang’s innovative procedure, second-stage reconstruction can be performed in approximately 3 months. - Stage 2 Silicone gel implant replacement and contralateral breast augmentation
When the tissue expander has dilated the breast skin and internal pocket enough to allow safe implantation after 3–4 months of saline injections, the second step, permanent silicone implant placement, can be performed. Dr. Chuang first removes the expander from the affected breast and re-dissects the existing pocket with ESUs and an endoscope; then, a silicone gel implant fitting the size of the pocket is placed. Perfectionist patients may also opt for endoscopic breast augmentation for the contralateral (normal side) breast to achieve symmetry and balance.
The two-stage procedure avoids risks associated with one-stage reconstruction such as capsular contracture, implant displacement or deformity, or wound healing. Breast skin would be more stable and less likely to contract after a period of expansion, which makes postoperative breast massage and maintenance easier. Patients also gain more time in considering their needs and do not have to limit the implant size due to skin elasticity. It is a more customizable surgery. However, it requires a longer waiting period to complete whole breast reconstruction. Excessive skin tension during the expansion period could also cause problems such as poor wound healing or infection. Moreover, the unilateral placement of expander usually temporarily affects the clothing choices of patients.
This surgery is not only suitable for those who have undergone sub-total or total mastectomy with radiation therapy due to breast cancer but also for those with multiple lumps or breast deformity due to PAAG or silicone injections, Dr. Chuang also recommends undergoing total or subtotal mastectomy combined with the implantation of a saline expander in the first stage and waiting for 3–6 months before the second stage to ensure the safety and efficacy of the entire procedure.
Surgical coditions
Stage 1 Duration
- Type of anesthesia: General anesthesia
- Type of incision: Through an original incision scar from mastectomy
- Recovery: Within 2–3 days
- Removal of stitches: 7–10 days
Surgical coditions
Stage 2 Duration
- Type of anesthesia: General anesthesia
- Type of incision: Through an original incision from mastectomy (side of breast reconstruction), Periareolar or transaxillary (side of breast augmentation)
- Recovery: Within 3–5 days
- Removal of stitches: 7–10 days
General instructions
No food and water on the day of surgery
- Breast massage and heavy compression should be avoided after the implantation of the expander in the first step.
- Postoperative massage should be performed for at least 6 months after the second step of reconstruction.
- Tasks and exercises that require excessive arm strength should be avoided for 1 month postoperatively.
- Underwired or push-up bras should not be worn for 3 months postoperatively.
Ideal candidates
- Those who underwent total or subtotal mastectomy.
- Those who underwent radiating therapy after mastectomy.
- Those who need mammary gland removal due to lumps from PAAG or silicone injections.
- Those with tight chest skin or scar contracture due to a severe burn injury.
- Those with chest skin thinner than 1 cm.
Possible complications
- Expander leakage
- Infection
- Poor wound healing
- Capsular contracture
- Implant displacement
- Implant rippling or wrinkling
- Numbness in the front chest
Surgical advantages
-
Staged surgery ensures the safety and efficacy of breast reconstruction.
-
Gradual expansion of chest skin with saline injections is beneficial for larger implants.
-
Breast skin is stabilized by expansion, which reduces the chance of capsular contracture or implant displacement.
-
Easier postoperative massage care; softer breast texture.
-
Can be performed with contralateral breast augmentation to increase symmetry.
-
More customizable; patients can be free to choose smooth or textured implants for the two-stage reconstruction.
Surgical drawbacks
-
Longer reconstruction and waiting period.
-
Monthly saline injections and concerns about possible leakage or infection.
-
Temporary dressing issues during the unilateral breast expansion period.
-
Higher cost than the one-stage reconstruction.