Subcutaneous Mastectomy
Because approximately 70% of gynecomastia cases stem from unexplained mammary overdevelopment or mammary proliferation (glandular type) induced by an endocrine disorder, internal medicine diseases and the feasibility of treatment should be first excluded prior to the operation. The chests of such patients feel relatively tough and predominantly composed of mammary tissues at the inside (mammary proliferation), which are difficult to be corrected by a single liposuction and mostly require subcutaneous mastectomy. Technically, a semi-circular incision is made at the periphery of the areola, via which the mammary gland is subcutaneously separated. Then, a majority of hyperplastic mammary tissues are dissected, and an average of 80–90% of mammary glands are removed to restore chest flatness, but a small part of mammary and adipose tissues should be preserved to avoid breast depression postoperatively. This surgery is conducted along with peripheral breast ultrasonic liposuction or regional breast skin excision sometimes to redress severe breast hypertrophy and sagging. Resected mammary glands are routinely submitted for pathological inspection to further confirm the presence of tissue abnormalities or possible lesions.
For patients with severe breast tissue proliferation like the female breast, performing mastectomy alone causes chest skin looseness and sagging, which undermines patients’ self-confidence, so Dr. Chuang recommends further total mastectomy and concurrent partial breast skin excision through an inferior margin incision to remove subcutaneous mammary tissues and tightens the chest skin. This male breast reduction surgery not only improves the appearance and symptoms of gynecomastia but also simultaneously smooths the anterior chest contour to restore the normal appearance of the male chest.
Surgical conditions
Duration
- Type of anesthesia: IV sedation + local anesthesia or general anesthesia
- Type of incision: A 2.5-cm incision at the inferior margin of the areola or a 5–8-cm incision at the inferior breast margin
- Recovery: 5–7 days
- Removal of stitches: 7–10 days
General instructions
No food and water on the day of surgery
- Avoid strenuous upper breast or arm activities for 1 month postoperatively.
- Wear tights or a chest girdle for 2 months postoperatively to fixate the breast skin.
- Take care of the scar frequently for 3 months postoperatively.
Ideal candidates
- Patients with idiopathic gynecomastia
- Those with mammary proliferation due to an endocrine disorder
- Those with abnormally hypertrophic or tough mammary glands that need to be excluded of breast lesions
- Those with mammary gland hypertrophy and milk lactation
Possible complications
- Subcutaneous seroma
- Hematoma
- Chest depression
- Scar proliferation
- Nipple hyposensitivity
Surgical advantages
-
Mammary glands are nearly completely removed, so there is no probability of proliferation in the future.
-
If effectively corrects the disturbance of lactation.
-
It radically dispels concerns of future mammary lesions.
-
It offers a more significant improvement than single breast liposuction.
Surgical drawbacks
-
The surgery is relatively extensive, and the recovery is slow.
-
A scar may be left at the periphery of the areola or interior breast margin.
-
Excess mastectomy may lead to breast depression.
-
Nipple sensitivity may be affected.
Possible procedures in conjunction
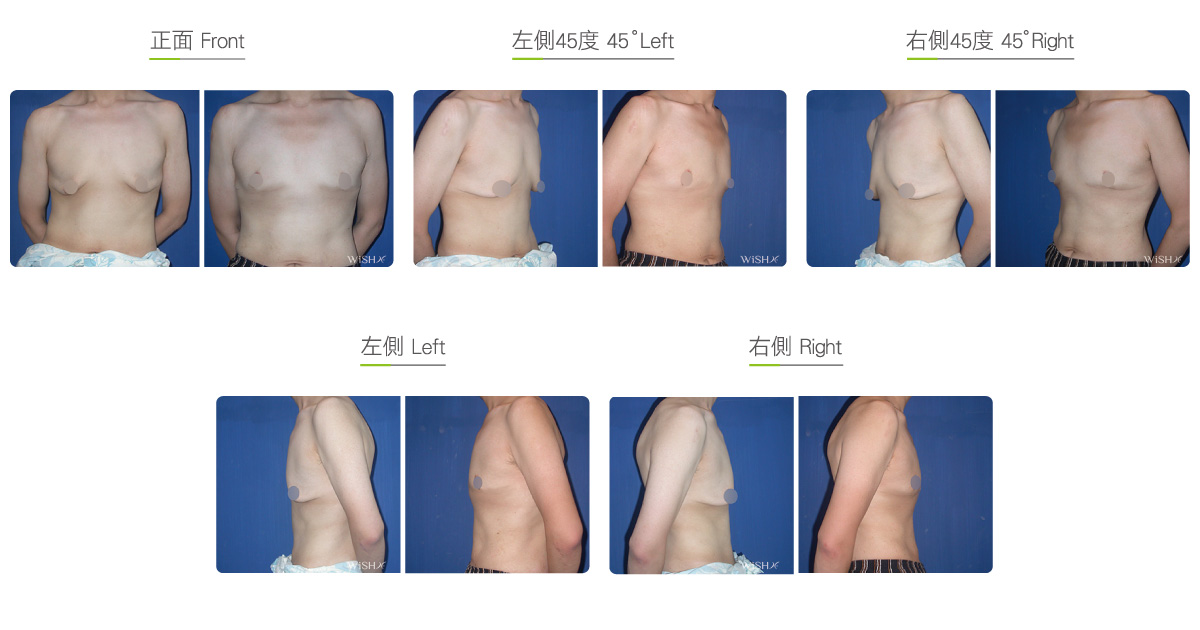
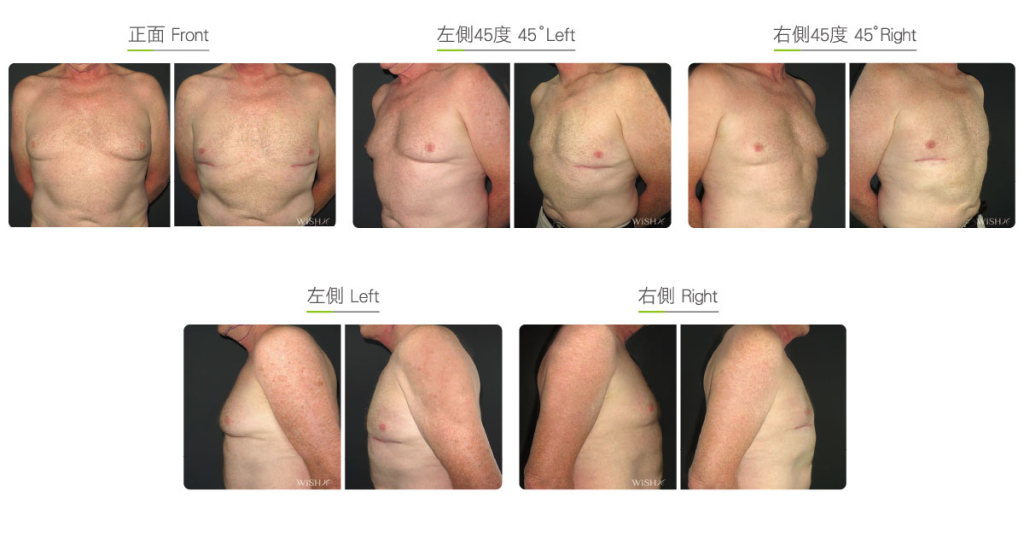
Before & After
Subcutaneous Mastectomy